You May Have Foot Bursae That Others Do NotSince the feet take such a tremendous load as we go about our daily tasks, there are several points in the foot that can develop bursitis due to added pressure and rubbing. As we stated earlier, the main bursae in the foot that become affected by bursitis include the metatarsal bursa, the metatarsophalangeal bursa, and the calcaneal bursa - BUT - other bursae can and will develop (and possibly become inflamed) where the foot requires excess cushioning. There are a myriad of interesting characteristics of the human body that are not well known, and the fact that the body will grow a bursa wherever it is needed is certainly one of them. Perhaps someone that frequently wears high heeled shoes over a long period of time will have bursae in areas that others do not. Another example would be someone that walks with an abnormal gait - over time bursa sacs may develop in areas where they do not develop in someone with a uniform gait. Common Bursae of the FootMetatarsalThe metatarsal bursa is located at the base of the toes on the bottom of the foot. This bursa can be irritated when one metatarsal bone takes more load than the others. When this happens, the soft tissue between the bone and the skin becomes compressed and inflammation in the bursa can begin. Walking barefoot on a hardwood or tiled floor without cushioning will increase pain noticeably due to the direct pressure on the metatarsal bursa. Bursitis can occur on the top of the toes as well. Those suffering from conditions like hammertoe often develop bursitis as a secondary condition. An abnormal toe joint can cause excessive rubbing against shoes. The constant rubbing will make the toe tender, swollen and red as bursitis sets in. Wearing shoes is painful and even the pressure from wearing socks can cause pain and discomfort. 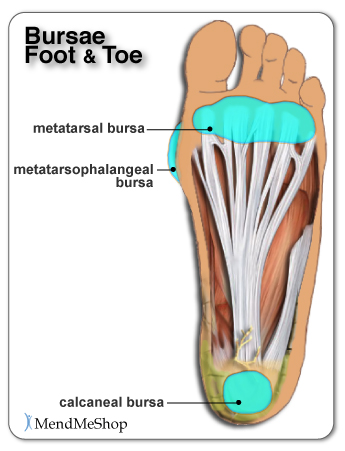 IntermetatarsalIntermetatarsal bursitis occurs when the tiny bursa between the toes (metatarsals) become compressed. Tight and narrow shoes can be the cause, however, it can occur naturally as we age and the arches in our feet begin to flatten. As the arches fall, the metatarsals put more pressure on the bursae that separate the toes. In this situation, swelling is rare but the pain usually travels right up to the toes. Wearing wider shoes and supports in your shoes can decrease the pressure on the bursae and help to alleviate pain. MetatarsophalangealThe metatarsophalangeal bursa is located on the inner part of the foot near the big toe. This bursa is a common spot for bursitis to develop as it is where a bunion (enlarged metatarsal bone) causes excess rubbing. Naturally, a bursa by a bunion can become inflamed with the excess friction in the area. Patients suffering from bursitis in the metatarsophalangeal bursa often have difficulties finding shoes that do not exacerbate the pain and sometimes resort to open shoes that do not cover the painful bursa. CalcanealAt the bottom back of the heel lies the calcaneal bursa. Bursitis is common in this bursa due to the thinning of the fat pad in the heel over time. The micro-trauma the heel undergoes with every step eventually becomes too much and the bursa becomes inflamed. This type of bursitis can be difficult to treat due to the constant pressure on the heel. Without proper rest and rehabilitation, bursitis may become a chronic problem in the heel. Heel cushions and prescription orthotics with extra foam in the heel can help to relieve the pressure but as with other types of foot bursitis, conservative treatment methods are recommended for a faster recovery and to prevent bursitis from becoming a life long nuisance. 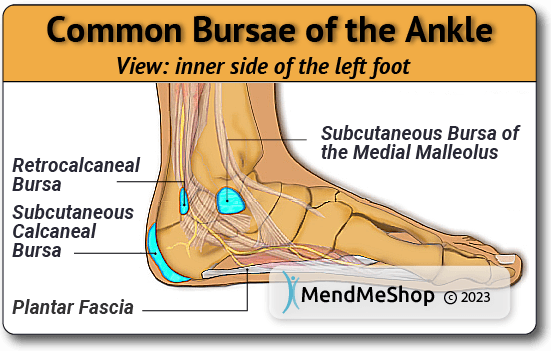 Symptoms of Foot BursitisThe most recognizable sign of foot bursitis is swelling caused by the enlargement of the bursa. This swelling is the build up of excess fluid in the bursa.  When you suffer from bursitis you typically feel significant pain in the area of the inflamed bursa. If tendonitis is also present, the pain can radiate away from the bursa. Direct pressure on an inflamed bursa will increase the pain and should be avoided if possible. You may also experience weakness in tendons and muscles surrounding the bursa as the pain worsens and inflammation in the area spreads. As the bursa becomes more inflamed you will experience swelling, tenderness, warmth & redness. In severe cases the bursa will appear as a bump and is usually red, appearing extremely tender and painful. Swelling can cause difficulties moving your toes, foot, or ankle as the range of motion in the joints of your foot will be affected. Swelling may appear immediately following trauma, over a couple of hours, or up to 7-10 days after the event that caused the irritation. You will most probably be limping from the pain. It is important to treat bursitis in the early stages to reduce the symptoms, minimize damage and maintain motion and strength in your foot. Resting your foot, using proper cushioning and comfortable footwear, and reducing any activities that add pressure on your bursa will help to reduce your pain and bursitis inflammation. When at rest, the fluid in the bursa decreases, helping to relieve the pressure and pain. By treating your foot bursitis in the early stages with conservative treatment method, you are more likely to prevent long-term damage and chronic conditions from setting in. Causes of Foot BursitisBursitis is caused when an inflammation occurs and excess fluid builds up in one or several bursae. This build up of excess fluid can be caused by many different factors. The biggest factor is the bursa becoming inflamed due to strain or something (like a muscle, bone or tendon) rubbing against it too hard. High Risk - Pronation Abnormal pronation, or how much your foot rolls when you step, can cause the joints to move in ways they are not suppose to adding pressure on the bursae. This can cause irritation and inflammation and can start to cause pain in the bursae as well as in the surrounding tissue. Twisting your ankle the incorrect way or moving too quickly can cause the bursa to pinch resulting in an inflamed bursa sac as well.  Wearing uncomfortable or improper footwear throughout the day or while playing sports also increase your chance of bursitis developing in your feet and toes. Wearing proper fitting shoes with cushioning will make your feet feel better and reduce your risk of bursitis. Other causes of bursitis in the foot include:
Do You Really Have Foot Bursitis?Visiting your doctor when you have foot, ankle or heel pain is always recommended, as there are many possible issues that can happen within the foot. Sometimes, one set of symptoms can result in multiple diagnoses. Some conditions that can show similar symptoms to various types of foot bursitis:Haglund's Syndrome This condition that occurs at the back of the heel when you are suffering from achilles tendonitis & bursitis at the retrocalcaneal bursa. The retrocalcaneal bursa is a small fluid-filled sac at the back of the calcaneus (heel bone) that allows the Achilles tendon to slide smoothly over the heel bone.  Haglund's Deformity is a painful, enlarged boney protrusion of the upper posterolateral calcaneus that is caused by calcification of the heel bone due to the inflammation of Haglund's Syndrome. Unfortunately, this boney protrusion causes further irritation to the retrocalcaneal bursa and achilles tendon due to excess compression of the Achilles tendon and bursa between the protrusion and the back of shoes or other footwear. This increased irritation then causes Haglund's Syndrome to become worse - thus completing a vicious cycle of 2 conditions causing each other to continuously worsen. 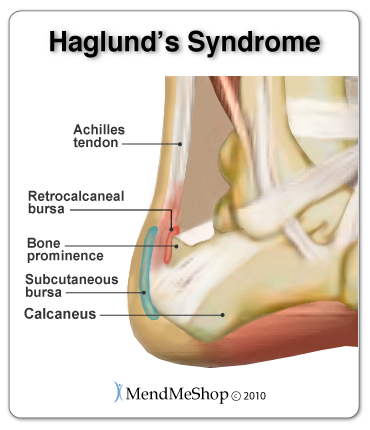 Morton's NeuromaMorton's neuroma will show symptoms of burning pain in the ball of the foot that may radiate into the toes. The pain generally intensifies with activity or wearing shoes. You sometimes feel that you are "walking on a marble," and you have persistent pain in the ball of your foot - you may even experience numbness in your toes. If you have Morton's Neuroma, you are experiencing a thickening of soft tissue that surrounds the digital nerve leading to the toes. This condition is caused by irritation, trauma or excessive pressure. Morton's neuroma most frequently develops between the third and fourth toes. MetatarsalgiaMetatarsalgia will show symptoms of pain in the "ball of your foot" - basically the area between your arch and the toes that supports your weight when your heel is off the ground. This ball-of-the-foot pain is often located under the 2nd, 3rd, and 4th long bones of the foot (metatarsal heads) or sometime more at the base of the big toe (1st metatarsal head). Metatarsalgia is a common overuse injury; persistent stress on the metatarsals can lead to chronic irritation and inflammation of the bone covering and surrounding tissues, such as ligaments and tendons. Increased risk of of metatarsalgia comes from:
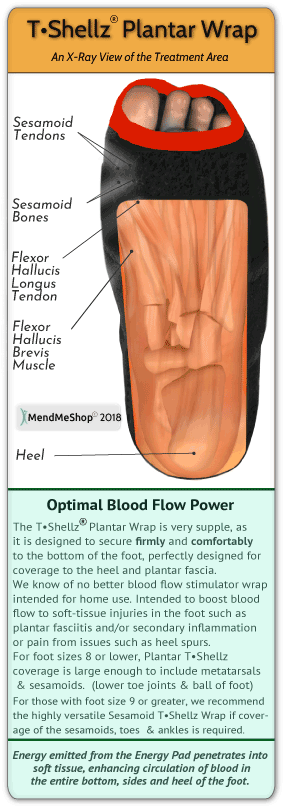
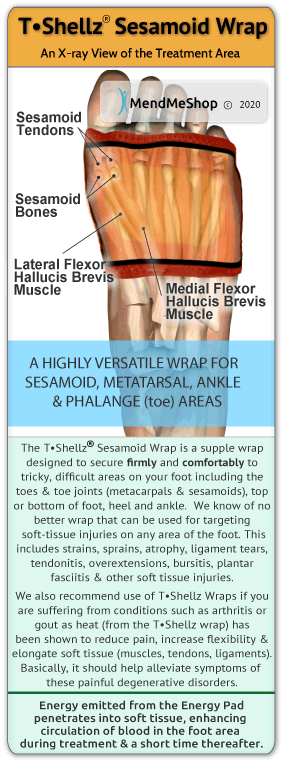
SesamoiditisSesamoiditis will occur when there is pain and inflammation in the sesamoid tendons that encapsulate the sesamoid bones. You may experience pain that will come and go in the ball of the foot just beneath your big toe joint. This pain will build-up over time rather than happen over-night. Swelling of the ball of the foot and bruising may or may not be present. You may notice range of motion changes and start having a hard time bending or straightening the big toe. 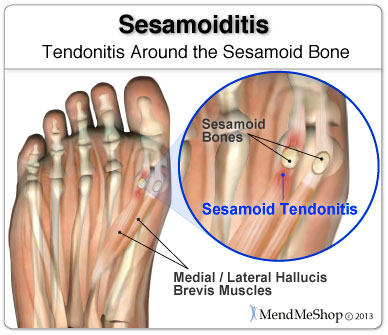 Plantar FasciitisPlantar Fasciitis pain associated with plantar fasciitis normally starts as a dull ache and then progresses to a sharp, knife-like pain or constant throbbing feeling that is worse when you put weight on your foot. The most tender areas tend to be in the center of your heel and along the inside and bottom of your foot towards your toes, where your heel and arch meet. It is worsened when you move your toes upward. Plantar Fasciitis is an inflammation of the Plantar Fascia, the tissue along the bottom of your foot that connects your heel bone to your toes, and supports the arch of your foot. How Do I Diagnose Foot Bursitis?When you are experiencing foot or heel pain and suspect you have bursitis, the best way to diagnose this condition is with a quick visit to the your doctor for a physical examination of your foot. Getting a proper diagnosis is important so you can treat your condition correctly. Untreated chronic inflammation of bursitis can lead to calcification of the bursa. Calcification of the bursa will mean that it will become more persistent and even more painful than before. To begin with, your doctor will gather a medical history about you and your current condition and symptoms. He/she will ask about the amount pain you are having with your lower leg and foot. How long you have had your symptoms and if you are experiencing a range of motion loss or limp when walking/running. Details about what caused the pain in the foot, when it started, and whether or not you have ever had treatments for this or a similar condition in the past, are very helpful in assessing your injury.  Range of motion movements / tests will be done to see how much movement has been lost in your foot. Your feet might hurt from the doctor poking and prodding at it, but by doing this the doctor will better understand the source of your pain, the level of tenderness in the area and how well you can move with this condition. Your doctor may also consider any previous foot/knee injuries or joint stiffness that you may have had in the past. This will help the doctor to determine if you have a more complex injury in your foot and rule out any other foot injuries that may be present.
If a soft tissue injury is suspected, an MRI may be undertaken to view where and how extensive the damage is. An x-ray may be recommended to rule out other possible causes of your symptoms. Possible causes of pain that an x-ray can identify include instability, abnormal bone shapes (bone spurs or bone cysts), wear and tear on the joints, avulsion fractures (when a fragment of bone tears away from the main bone along with the muscle, tendon, or ligament as a result of trauma), dislocations, arthritis, calcium deposits in the bursa or joint, and/or other problems. Some bursae in the heel are close to the surface of the skin and are more susceptible to infection (caused by a cut or scrape) than most other bursae. An infected bursa is known as "septic" and is something to take seriously as it can quickly become life threatening. Your doctor may aspirate (use a needle) to remove fluid from the bursa to check for possible staphylococcus epidermis (or staphylococcus aureus) bacterial infection. Your doctor will be able to determine whether there is an infection or not by drawing a small sample of the bursa fluid with a needle. If it is determined that your bursitis is septic, you will be prescribed antibiotics to get rid of the infection. A physical examination will be performed to determine if you have any signs of Achilles Bursitis or other ankle injury. He/she will look and feel the soft tissue and bones in your ankles and feet to note any differences between the two of them. This will identify any abnormalities, such as swelling, bone deformities, atrophied muscles, redness and/or warmth on the skin. In many cases, the first sign that you have bursitis is swelling, typically accompanied with significant pain. Foot Bursitis Home Remedy OptionsSuggest Conservative Home Treatments to Help |
                |