Bursectomy - Surgical Bursa Removal
Post-Operative Rehabilitation
Reasons for Undergoing Surgery
There could be a multitude of specific reasons for a physician to recommend surgery. From a more general standpoint, the physician will try to take into account ALL factors (pain, quality of life, surgery risk, etc.) in determining whether surgery is of net benefit to you. In some cases, this is a simple determination as surgery is often performed to save a life when it is apparent the patient will die without an operation. In other cases where there is a soft tissue injury, surgery is typically the final resort option when recommended conservative treatment options have failed to help.
 If you are undergoing surgery for a bursa injury that was non-life threatening (septic), it is most likely that your doctor has put you through a course of conservative treatments for at least six weeks. They do this because it is generally understood by doctors and surgeons that surgery will introduce more scar tissue into the area. This added scar tissue will be problematic, requiring more visits to your physical therapist (PT) and conservative treatment options post-surgery. If proper recovery protocols are not undertaken following the surgery, your joint could easily wind up in worse shape than it was before the surgery! This is why surgery is only performed as a last resort.
Most doctors, surgeons and orthopedic specialists will recommend conservative treatment methods for minor bursitis injuries before even considering surgery.
Some conservative treatment methods recommended include:
- Rest - This is important for initial healing because without an appropriate amount of rest you are at risk for increased inflammation, pain and re-injury of your bursa, tendon(s) & muscle(s) in the joint. Too much rest can also be harmful because joint immobility can actually cause more stiffening in the joint. This is why rest should be used when reducing initial pain and swelling, but should not be considered for more long-term conservative treatment.
- Avoid Activity that caused your bursitis. - While resting your injury it's also important to avoid all activities that may have caused your symptoms, including any repetitive movement. This may include reduced activities in your job if that has caused or worsened your bursa injury. Continuing on with regular activities can increase the severity of your injury, turning a mild to moderate case of bursitis into serious joint damage, affecting not only the bursa, but tendons and muscles as well. This will lead to a higher probability of surgery.
- Apply a Cold Compress or Ice Pack - The application of immediate cold at the onset of your injury (or during flareups) will allow you to manage pain while getting rid of swelling and inflammation.
- Use a TShellz Wrap® - You can use your own blood flow to maximize your rehabilitation, maintain healthy blood flow, decrease recovery time, and boost overall long term health in the treated area. In most cases, promoting blood flow will help to minimize the growth of scar tissue, increase flexibility and help reduce the risk of atrophy. Some of our clients have found that the use of a TShellz Wrap® is especially helpful in dealing with chronic tendon, bursa & muscle injuries or on-going pain and stiffness from a chronic soft tissue injury.
- PT and rehabilitative exercise under supervision of a PT or doctor. The intent of this is to provide you with increased range of motion, pain relief and strengthening of the soft tissue surrounding the affected joint. Remember: Surgery is typically the last resort. This means doctors or surgeons typically won't perform a surgery until they feel that their patient has put effort into treating their injury with conservative treatment methods. This includes 4 to 6 months of PT. If you haven't experienced any improvement in your condition during that time then surgery may be considered.
Effective Conservative Treatment Options
are Available
If you are not at the surgery stage and your physician has opted to treat your injury with conservative treatment options, then you will find that many of our customers have had great success treating themselves with the powerful conservative treatment products such as the TShellz Wrap®. When used as directed, it is our opinion that the TShellz Wrap® is a crucial part of a conservative home treatment protocol - a protocol designed to aid in the recovery process. In some cases, a dedicated approach to home conservative treatments might make enough of a difference that perhaps you will not need surgery after all. If surgical intervention is required, talk with your physician about using these same products for post-surgery recovery as they are intended to be highly effective for reducing post surgery inflammation, enhancing range of motion and minimizing scar tissue growth.
If Surgery on Your Bursa is Required...
If all conservative treatment methods have been explored and your symptoms (pain as well as limited use for daily activities) persist, then you will be considered a candidate for surgery. You and your doctor may decide to move forward and have you undergo surgery, which will trigger the next chapter of your recovery journey. Your post surgery rehabilitation efforts will have an important impact on how soon you can return to living and enjoying your normal daily life.
If possible, avoiding surgery is typically the best option. However in some extreme cases the bursa remains thick and swollen, causing chronic bursitis pain and in such cases, a bursectomy is often advised. Surgical removal of a bursa (a procedure called a bursectomy or resection of a bursa) may be necessary if the bursa has become chronically inflamed. The type of surgery you will have depends on the type of injury you're faced with.
Bursa Draining, Bursa Aspiration
Generally when it comes to bursitis surgery you'll be faced with options for non-invasive procedures or more invasive solutions. If it's possible to do a non-invasive procedure, your doctor may suggest a less aggressive procedure such as draining or aspiration of your enlarged bursa.
The hope is that the removal of extra fluid from your bursa will reduce your pain, but it may only be a temporary fix if the bursa sac has thickened walls and has chronic inflammation. The cause of fluid build-up will also require treatment with conservative treatment methods following the procedure.
Bursitis Aspiration Surgery
This procedure is most commonly used for elbow bursitis. Your doctor will use a syringe filled with liquid (1% lidocaine) to raise the skin over the bursa and to freeze/numb the area. Your doctor raises the tissue to protect the tendons and ligaments in the elbow. A new needle will then be inserted into the bursa to drain the fluid and reduce the over all size.
How Long Will It Take To Recover From A Bursectomy?
Incision wounds normally take about 10 days to heal but this can depend greatly on the type of surgery that was performed (arthroscopic vs open surgery). Most patients find significant improvement from about 6 to 12 weeks after the surgery. There are times, of course, where the area will become quite sore then go away again - this is often due to movement and stresses put on the post surgical area.*
(*"Trochanteric Bursitis Surgery Sydney NSW | Hip Injury Treatment Darlinghurst." Hipandkneesurgery.com.au. N. p., 2018. Web. 18 Oct. 2018.)
In most cases, a new bursa will grow back within a couple weeks after a bursectomy. The new bursa will most likely be healthy and will not have the pain and inflammation that may have been experienced with the removed bursa.
What Happens After Surgery is Done?
Ask any doctor and they'll tell you that the success of your surgery depends on your level of dedication to regular, at-home care of the area during your recovery. Nearly all of our bursitis post-op clients have achieved a successful recovery through regular use of a Cold Compress or Ice Pack and the TShellz Wrap® at home, in combination with their PT sessions.
Using conservative home treatments on a frequent basis (1 to 3 times per day) will lessen the chance and/or severity of joint degeneration and muscular atrophy during your rehabilitation process. Talk to your doctor or surgeon to determine when you can begin home conservative treatments in coordination with your PT.
Getting Started with Bursectomy Post-Operative Rehabilitation
If you've had surgery on your bursitis injury then your doctor will quickly get you on the path to rehabilitation. The aggressiveness of your rehabilitation efforts and your injury's ability to heal will depend on a variety of factors including (but not limited to):
- your age, overall health, and activity level
- the state of your bursitis injury before surgery (severe injuries like thickened bursa sac, tendon or ligament damage, an open wound, bone damage or fracture will require more intense surgery)
- the type of surgery you had
- how soon you need to return to normal activity
Know that no 2 rehabilitation plans are alike - The less invasive your surgery is, the quicker your road to recovery will be.
Proper post-surgery rehabilitation is very important, perhaps even more important than the surgery itself. Most patients can leave the hospital the same day, perhaps using crutches or a cane depending on the surgery location. You will be required to follow up with your surgeon and a PT and they will advise you on your recovery.
The goal of a rehabilitation plan is to manage pain and swelling while improving function, strength, and range of motion. Ultimately at the end of your recovery you'll regain strength and return to full activity. In order to achieve this you'll most likely spend a lot of time at a physio clinic after your surgery, but as your healing progresses, emphasis will be placed on your personal at home treatment. The success of your rehabilitation will depend on your dedication to working with your doctor and PT while managing your recovery on a daily basis at home.
Regardless of what type of surgery you've had (or even if you don't need surgery) your home recovery routine can be improved by controlling initial and ongoing pain/swelling, and increasing blood flow to soft tissue in the area so you can achieve long-term, positive results. This can easily be done by incorporating the use of a Cold Compress or Ice Pack and a TShellz Wrap® (after surgical wound has healed and swelling has reduced) into your routine. Consistent use of conservative treatment tools like these will decrease your time spent in recovery. Speak to your doctor, surgeon or PT about incorporating TShellz Wrap® treatments into your post-operative rehabilitation program to boost your overall recovery process.
As you maintain healthy blood flow circulation in your affected joint it's also important to keep moving. If you stop moving your joint will stiffen up and surrounding muscle and soft tissue will begin to atrophy (waste away). You can strengthen your joint, muscles and soft tissue in your hip, knee, ankle and foot after bursitis surgery by incorporating a light stretching routine (assigned by your PT and/or surgeon).
Only AidMyBursa offers this recovery process that gets you on your feet faster, speeding up your overall healing with long-lasting, sustainable results.
Post-OP Phase 1: Protect Your Surgery Site & Start Moving
The level of protection needed will depend on the type of surgery you have had. Generally, for arthroscopic and open release surgeries, you may need to wear a sling(shoulder,elbow), brace or cast (knee, ankle, foot, wrist) for at least a week after surgery, or until your first follow-up appointment with the surgeon. You may be advised by your physician not to drive or operate a motorized vehicle for at least a week after your surgery. This is because restriction of movement may directly affect your ability to steer your vehicle, particularly in an emergency situation which may require rapid, deliberate movements.
Rehabilitation after surgery will first focus on protecting the area and initiating simple movement. Start doing simple movements to gain motion, preventing scar tissue formation which might limit your range of motion and cause further damage to soft tissue.
Directly after your surgery has been completed, you will undergo Step 1 of the healing process by stopping the bleeding that has started because of the incisions and work done on the bursa and surrounding area. Depending on the type of procedure you have just had, your tissue may be sutured together, reconstructed or removed to fix your underlying condition. In any case, as with any injury to soft tissue, the tissue will be bleeding again. Depending on the type of injury you have, your surgeon may even stimulate bleeding during your surgery to trigger the healing process.
 Typically, your body will have begun to stop the bleeding as soon as your surgeon has completed your surgery. This means that the veins carrying your blood will close off, and your blood will coagulate (condense to seal the bleeding off) in order to reduce the amount of blood loss in your body. Your body knows to do this automatically because blood is so vital to the healing process. Blood is basically the vehicle for oxygen and nutrients that travel directly to your soft tissue - where these things are needed most.
In order to reduce pain, swelling and inflammation, your doctor will prescribe an anti-inflammatory drug to be taken during the first week after your surgery, or for however long it is needed, depending on your pain level. Your surgeon will also recommend the use of a Cold Compress or Ice Pack on a frequent basis - multiple times per day - to control your inflammation and reduce your pain.
If you have undergone an arthroscopic surgery, you may have less blood loss and your doctor or surgeon will check before you leave the hospital to make sure your bleeding at the incisions has stopped. If you have undergone open surgery, your doctor and/or surgeon will check your incisions periodically over the next few days of your hospital-stay to ensure that your body has stopped the bleeding on its own and also make sure that your incisions are starting to heal.
Movements to Watch Out For After Surgery
Depending on the joint that was operated on, you me be advised by your physician NOT to drive or operate a motorized vehicle for at least a week after your surgery. This is because you will have still have limited range of motion. However, for elbow or shoulder surgery, you are probably finding it difficult - if not impossible - to drive anyway... so this shouldn't surprise you.
Right after surgery, avoid straining the joint that was just operated on.
Do not lift heavy objects and try not put any strain on the joint for four to six weeks following surgery - this may include using a keyboard / mouse, mobile phone, climbing stairs, and even dressing.
Sleeping may provide a challenge for quite a few people. For elbow or shoulder surgery, try putting a towel roll under your elbow to support your arm. Adding an incline wedge to your bed may be more comfortable than lying flat.
For sleeping after knee surgery, it is recommended to:*
- Sleep on your back (not your stomach)
- When sleeping on memory foam, use a pillow or foam wedge under your knee
- Don't sleep on your stomach
- If you sleep on your side, sleep on the side that was not operated on with a pillow or two between your legs to keep your recovering knee stable
- A recliner or zero gravity chair will provide good knee support & promote good blood circulation while keeping your knee stable.
(*Ellis, N., Ellis, S., Ellis, Nicky et al. "The 3 Best Sleeping Positions After Knee Arthroscopy." We Sleep Well. N. p., 2018. Web. 19 Oct. 2018.)
For sleeping after hip surgery, it is recommended to:*
- Sleep on a firm bed or mattress.
- Use a pillow between your knees
- Don't sleep on your stomach
- Don't sleep with pillows beneath your knees
(*"Sleeping After Hip Surgery | Cleveland Clinic." Cleveland Clinic. N. p., 2018. Web. 19 Oct. 2018.)
Your surgeon may instruct you to wear a sling/cast/brace/walker at all times for 4 to 6 weeks. The length of time needed will depend on the type of surgery you have had. You may remove the sling/brace/cast for exercise as prescribed by the surgeon or therapist, icing, dressing and showering. Normal daily activities around the house and/or work activity may be considered acceptable as long as you wear the sling/brace/cast.
After your incisions and repaired/removed soft tissue have stopped bleeding, the area will probably be tender, swollen, red and hot to the touch - these are all symptoms of inflammation. Step 2 of the healing process is inflammation reduction. At this point you will be home if you have had arthroscopic surgery, or you may still be in the hospital if you have had open surgery. In order to reduce pain, swelling and inflammation your doctor will prescribe an anti-inflammatory drug to be taken during the first week or 2 after your surgery. Your surgeon will also recommend cold and compression, like R.I.C.E. (Rest, Ice, Compression, Elevation).
Rest at this point is vital to your rehabilitation plan depending on the surgery you have undergone. If you have had arthroscopic surgery with minimal internal wounding from your surgeon, you may be encouraged to start movement early or as soon as possible. Limited movements of the joint will be required in most cases after the surgery. If you have had an invasive open surgery, then you may be encouraged to rest longer at first before starting movement.
Your doctor or surgeon will advance you to the next Phase of rehabilitation when there is no evidence of inflammation or swelling in the joint. If you have had arthroscopic surgery, your doctor may expect that you are able to move your joint around pain free before moving onto the next Phase of rehabilitation.
Post-OP Phase 2: Gain Back Range of Motion (ROM) and Stability
After the initial healing from your surgery, your soft tissue will be in a weakened state and will not be as strong as healthy tissue for some time. This is why you need to be on "re-injury watch" and make the most of your home therapies and PT appointments during your rehabilitation. It would be devastating if overdoing it at any point during the first few weeks or months of rehabilitation, would send you right back into the operating room.
When Step 1 and 2 of the healing process is done (phase 1 complete), temporary tissue will start to grow around soft tissue that was damaged during your injury or the surgery. Step 3 is the Growth of Temporary Tissue.
Once your new tissue has begun to grow you will be encouraged to gain back some of your range of motion (ROM) and increase the stability of your joint. Depending on the location and severity of the surgery, your doctor or surgeon may also introduce regular PT appointments (generally within 2 to 6 weeks after surgery). You may still be expected to wear a sling/cast/brace to reduce the amount of stress you are placing on your joint during movement (reducing your risk of re-injury).
You will start gradual movement of your joint in a free (non-forced) way with very low impact exercises, normally with very few repetitions of activity. Your joint may be stiff at first, and you should expect simple and easy movement to be a bit more difficult for you to master and painful. Exercise of any kind is a method of increasing blood-flow in your joint to increase the amount of oxygen and nutrients that travel to your injured tissue.
You might start with gentle active limb extensions and flexion exercises with a hard brace/cast on at 0 - 14 days. In weeks 2 & 3, when you're out of a hard brace, pain is the guiding factor with tolerance of weight-bearing for any exercises.
Strengthening exercises will slowly increase in difficulty (with more resistance) around 3 - 8 weeks after your surgery.
If your bursa surgery involved tendon repair, at about 6 to 12 weeks (depending on your type of surgery) you still need to allow for healing from the surgery. Although you may be feeling much better and your pain is reducing, your joint at 4 weeks will typically be healed less than %30. At 8 weeks it will be about 40% strong and after 12 weeks the tendon is 60% as strong as normal tendon. The point where the pain decreases yet the tendons are still weak is a critical point - this is the stage where you need to be very careful about re-injury.
Your surgeon will recommend regular PT appointments in the first 6 weeks after surgery. The type of surgery and the degree of damage to your joint will also make a difference in how soon you start PT.
Your PT appointments will be 1-3 times per week, and your progression of movement in your joint will be the guide. At your appointments you will be encouraged to gain back some of your range of motion and increase the stability of your injured joint. You will start with the gradual movement of your joint in a free (non-forced) way with little weight or resistance, normally with very few repetitions of activity. Your joint will be stiff and painful at first, and simple movements may seem challenging in the beginning. Don't be discouraged, your hard work will payoff in the end!
At Home Stretching/Exercise - Your therapist will encourage you, telling you just how important it is to commit to regular exercise at home as well as in the clinic. You should be doing homes exercises up to 3 times per day. They will give you the exercises and guidance based on your overall soreness level and your morning discomfort.
We advise that you apply a TShellz Wrap® treatment to help increase your blood flow before stretching (or exercise). Apply a TShellz Wrap® treatment for approximately 15 minutes (finishing 15 minutes before exercise) to help increase elasticity and flexibility of tight tissue in the treatment area. The increased elasticity will help minimize tissue tears and scar tissue growth (increase ROM and decrease re-injury risk.

Controlling post-exercise swelling and inflammation is crucial during this Phase. Any sign of swelling or inflammation after exercise may be an indication of minor re-injury to soft tissue in the joint. Control your inflammation immediately after exercise with a 15 to 20 minute cold treatment. If you are not careful to treat your swelling or inflammation immediately after exercise, you may experience a set-back in your recovery.
Your doctor, surgeon or PT will advance you to the next Phase of rehabilitation when you show measured improvement of range of motion (ROM), strength, stability and flexibility of your joint. The level of improvement will depend on the severity of your injury and the type of surgery you have had. For example, if you have had a relatively simple arthroscopic repair of tissue, you may be expected to move the joint around before moving to Phase 3 of your rehabilitation.
If you have questions, call our office at 1-866-237-9608 (toll free continental US).
Post-OP Phase 3:
Gain Back Full Capability of Your Joint
After temporary tissue has grown (Step 3 of the healing process), this temporary tissue will go through different stages of conversion into healthy, normal, flexible tissue. This is Step 4 of the healing process (Complete Tissue Re-Growth). Before converting into healthy tissue, temporary tissue will often become tough, dense, fibrous scar tissue. Scar tissue has an unorganized, inflexible tissue structure, which makes it brittle. Scar tissue will provide your injury with more long term fusing power, but will also stick to surrounding healthy tissue. The growth of this scar tissue is what stiffens your joint, restricting movement and flexibility.
This phase of your rehabilitation will focus on an increase in activity level in order to regain full range of motion (ROM) and muscle strength in the area of the surgery. Your doctor or PT may increase your activity by introducing the regular use of a rowing machine, weight press or pull-down machines.
We generally recommend clients to consider using a TShellz Wrap® BEFORE workouts and a Cold Compress or Ice Pack after work-outs. This protocol will go a long way to maintaining overall tissue stretchability, reduce re-injury risk, and treat any pain, swelling or inflammation due to overexertion of the joint.
Your doctor or PT will advance you to the next Phase of rehabilitation when you have regained full ROM (range of motion) without pain in your joint. You may also have to pass clinical exams or tests of your muscle strength, balance, stability and flexibility in order to be cleared for Phase 4.
Post-OP Phase 4: Return to Regular Use & Activity
Depending on your job (and whether your occupation has contributed to causing your condition), you may be able to return back to work from within 6 to 12 weeks after the surgery. Overall healing of the joint after surgery may take upwards of 6 to 12 months, which means you may not be able to return to sports or do heavy, forceful activities until a year has passed after your surgery.
In many cases, your doctor or surgeon may recommend that you continue muscle strengthening and stretching instructed during your rehabilitation in order to maintain healthy ROM. Additional cardiovascular exercise will also be encouraged. If you are an athlete or have a job that requires extensive physical capability, your doctor or PT will likely advise a very gradual return to previous activity. They also may encourage continued rehabilitation and/or maintenance of your joint through PT or conservative treatment methods, to prevent re-injury.
Scar tissue may plague you for weeks, months and maybe even years after your surgery depending on your level of activity and the amount of conservative treatments you have undergone during your rehabilitation. Scar tissue will be a major problem as scar tissue can easily build up quickly and its hard to get rid of.
Even if you have been cleared to get back to activity, you still must be careful with the activity you take on. You need to keep in mind that your joint won't be back to 100% for some time (if at all) and so continued stretching with exercises and stretches and treatment with T•Shellz and cold will maintain good health of the joint and significantly reduce your risk of re-injury.
Dealing with Scar Tissue After Surgery
How Scar Tissue Affects Your Rehabilitation
Tendons, ligaments, muscle and other soft tissue in the joint are all meant to be soft and flexible, ready to work and move small to extreme forces in everyday activities. When I say extreme force, I mean try to imagine the amount of tension that is put on your ankles, hips and knees when running or climbing stairs - even when you are just walking even, let alone running. Shoulders and elbows often deal with heavy or repetitive forces at work if you are a tradesman, garden or work in an assembly line. Try to imagine the amount of force that your arm puts on your elbow and shoulder when you are just trying to throw a football or lift something heavy.
Scar tissue grows in damaged tissue when it tries to heal; little tiny band-aids that overlap each other to bind tiny tissue tears together. With this added scar tissue, muscles & tendons & ligaments become rigid, less flexible and unable to handle the forces that it once could. If scar tissue is found in a bursa, this can impede joint movement and/or cause pressure points - increasing the risk of further soft tissue injuries and inflammation. If you're suffering with scar tissue now you may feel the effects with stiffness, tightness, weakness and tiredness in your joint and muscles.
Scar tissue can form fast to bring together the edges of a tear, but working fast doesn't mean that the job's done right. When scar tissue forms it doesn't come together as neatly as regular (healthy) tissue would. Scar tissue fibers will lay down over top of your tear in a cluttered, messy and jumbled up way.
On-going issues with scar tissue can result in soft tissue tears and increase chances of strain to nearby tendons or ligaments (as they are now handling higher forces due to overcompensation).
Scar tissue is one of the MAIN reasons why a chronic soft tissue injury has not healed and your Range of Motion (ROM) is reduced from what it once was.
Scar tissue will form fast to deal with a soft tissue injury, and this scar tissue will attach to EVERYTHING in the area, including the surrounding healthy tissue as well. This can result in a fusing together of soft tissue that shouldn't be fused together (muscles,tendons,ligaments), and this will cause extreme pain when you move your leg - it is literally ripping scar tissue. This is why PT is often painful - the therapist stretches the joint, forcing the scar tissue bonds to break so you can regain your range of motion.
Scar tissue can become a major problem and cause your injury to become chronic - taking months or even YEARS to completely heal!
Scar tissue is something that will be present in and around your bursa before and after your surgery. The growth of scar tissue is ultimately what causes stiffening in the joint, restricting movement and flexibility. Scar Tissue is something that cannot be avoided during surgery. Your surgeon will determine if the anticipated outcome from surgery will be successful, despite the buildup of scar tissue that you will develop as a result of the surgery. Overall, the surgeon may be able to remove a lot of the initial buildup of scar tissue around the injury and in doing so, view a positive outcome from the surgery.
You can quickly minimize scar tissue growth and reduce risk of re-injury by increasing blood flow and adding heat to the area. Both of these attributes when combined with a stretching plan will certainly help stem the rapid growth of scar tissue. Treating yourself with a TShellz Wrap® is the easiest and most effective way to achieve both an increase in flexibility/elasticity while also triggering the body to maximize its potential to heal quickly due to the substantial increase in blood flow.
Unfortunately, scar tissue may plague you for weeks, months and maybe even years after your surgery, depending on your level of activity and the amount of conservative treatments you have done during your rehabilitation. Scar tissue can become a major problem in a short amount of time.
Your Success To Recovering From Bursa Surgery Is Largely Up To You
- Listen well to your physician and remember to stick to your home conservative treatment plan. Doing this consistently, every single day will help you minimize the amount of scar tissue that will grow in the wound and maximize your opportunity for a healthy recovery.
- know that frequent use of a
Cold Compress or Ice Pack after surgery will help reduce the swelling very quickly. Most of the pain you usually feel will be from the swelling, and you'll be surprised how fast pain drops once the swelling is down. Scar tissue growth is further inhibited by a reduction in inflammation (swelling restricts blood flow - tissues die without blood and scar tissue grows in its place)
- know that the
TShellz Wrap® will help reduce scar tissue and increase blood flow to the area. Treating your joint with this device after surgery should become a vital component of your home conservative treatment protocol. (Do not use if there is a lot of swelling or the incision site has not healed yet and only once you assigned stretches for home - generally at least 6 weeks after)
- use the
TShellz Wrap® before physical activity.
Circulatory Boost treatments increase flexibility and elasticity of soft tissue, improve range of motion (ROM), reduce stiffness and tightness and reduce the chance of tissue strain during activity.
Scar Tissue & The Bursa
Even when you're injured and in pain you need to keep moving to break up scar tissue that's forming around your bursa. Moving when you're injured is hard. Since moving while injured can be painful - most people think it's better to stop moving, rest their body and hope that their bursitis will heal all on its' own after surgery. Even though rest is important to recovery too much rest during the recovery process will increase the amount of scar tissue in your joint.
During the healing process your body will fill in tears in your soft tissue and bursa sac with dense, brittle tissue called "scar tissue". This process is no different after you've had surgery to remove your bursa or drain fluid from your joint. The human body will use scar tissue as a temporary solution and will try to build the scar tissue as fast as possible to heal the area. Scar tissue can form fast to bind everything together in your joint, but working fast doesn't mean that the job's done right. When scar tissue forms it doesn't come together as neatly as regular (healthy) soft tissue would. Scar tissue fibers will lay down over top of the damage in and around your bursa in a cluttered, messy and jumbled up way.
Imagine throwing a bunch of drinking straws in the air... Those straws will land in a random, unorganized way. It seems silly to think that those straws could land perfectly straight and all in the same direction.
This is how scar tissue works. The scar tissue that forms on your bursa will be unorganized and won't line up properly with the healthy tissue surrounding your joint. This scar tissue will also attach to everything in and around your bursa, including the surrounding healthy tissue as well. This can result in a long-term fusing together of your tissue that stiffens up your entire joint, reducing your mobility and making your bursitis injury even more painful!
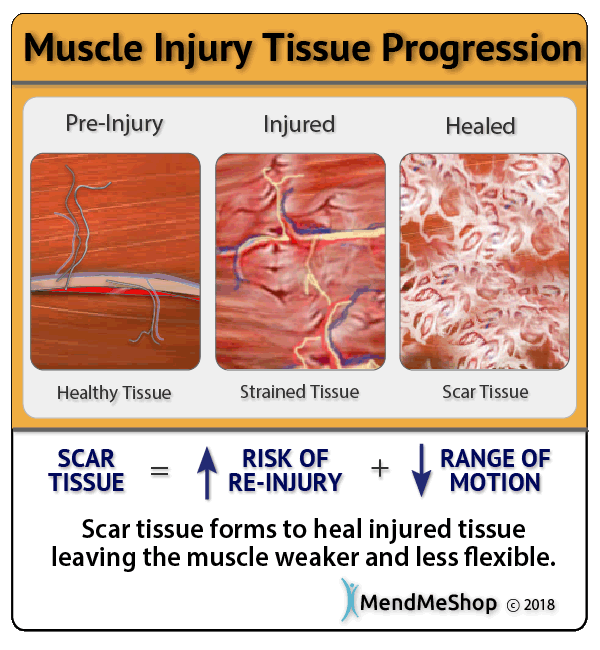
This is why scar tissue is weak and only a temporary solution to heal your bursitis injury. Scar tissue is something that needs to be dealt with fast. If you try to get back into your regular daily activities after surgery with a mound of scar tissue in your joint you'll have a higher risk of re-injury and also overcompensation injuries. Scar tissue is just not built to withstand the pressures of regular activity.
If you have an injured bursa with a lot of scar tissue and re-injure that tissue, even more scar tissue will grow to fill in those tears. If you keep falling into the dangerous cycle of re-injuring your bursa without proper treatment you could end up with massive amounts of scar tissue in your joint. Your ability to move your affected joint in a normal way will be impaired as the amount of scar tissue increases.
The only solution to truly recover from invasive surgery for good is to break up scar tissue and avoid re-injury.
This can be achieved through regular use of the TShellz Wrap® accompanied thereafter with light stretching. A light consistent stretch regimen will help break down scar tissue and improve flexibility during your post-op recovery.
Expectations for Long-term Recovery
Rehabilitation after bursa surgery is just the beginning of your recovery process. Even after you've had surgery to fix the problem and deal with the build-up of scar tissue, it is improbable that your soft tissue will heal 100%. From this point forward, it is more important than ever to be careful with the joint that was recently operated on. The joint is probably weaker now, and your risk of re-injury is much higher because of this.
Manage your symptoms on a daily basis to Reduce re-injury Risk
It is generally not difficult to manage a long-term healthy recovery from surgery with conservative treatment methods that can be used in the comfort of your own home. If you're looking for an all-natural form of pain management and a Localized Enhanced Circulatory Response mechanism for long-lasting relief, seriously consider the benefits of incorporating the TShellz Wrap into your treatment plan.
A Cold Compress or Ice Pack can help you to decrease post-operative pain and swelling while also managing any pain from occasional inflammatory flare-ups (re-injury). Consistent treatment with a Cold Compress or Ice Pack will reduce inflammation and gently numb nerve endings in your tissue for effective pain relief after injury flare ups.
During your last few stages of rehabilitation, while you're undergoing PT and focusing on improvements to your range of motion, it's important to maintain healthy blood flow in your hip. Strong and healthy tissues need a solid local circulatory system, and this is exactly what our TShellz Wraps are made for.
Reduced blood flow slows down your recovery process. If your tissue remains in this condition, you'll always be at risk of re-injury that will severely set back your healing progress.
Use TShellz Wraps regularly to prevent re-injury and keep your muscles, tendons and ligaments elastic and flexible. Healthy blood flow is vital to the healing process after hip surgery. Your blood flow is what brings oxygen, nutrients and energy (things needed to heal) into your damaged tissue. Blood Flow promotes tissue re-growth, strengthening the delicate work your surgeon has done.
Regular treatments with the TShellz Wrap® will help you increase blood flow for up to 4 hours with just one 20 minute application. The TShellz Wrap® is intended to (1) increase blood flow in the treatment area and (2) increase the length and elasticity of soft tissue. Both of these qualities together provide long-term soft tissue health benefits while reducing the risk of re-injury and overcompensation injuries.
Use a TShellz Wrap®:
- After swelling and inflammation have been reduced with cold compression.
- BEFORE getting out of bed in the morning. BEFORE going to bed at night.
- BEFORE exercise, workouts or activity of any kind to increase elasticity of tissue in the area which in turn reduces your risk of further injury/re-injury.
- Anytime you feel your bursa site may have stiffened up, is tight and your mobility is reduced causing you more pain.
- Anytime you have sore or aching tissue as long as there is not substantial swelling.
- AFTER surgery (once the skin wound has healed over and swelling has reduced - basically at least 6 weeks after the surgery) to boost blood circulation, helping surgically repaired tissues recover for long-term health and minimize scar tissue growth at the surgery location.
- Anytime BEFORE you feel you might undertake activity that will put significant strain on the injury area.
- Any other situation where you need to increase blood flow to relax your tissue, relieve pain, prevent re-injury and enhance flexibility in the area.
When to use a Cold Compress or Ice Pack:
- 24 to 72 hours after your initial injury or when you first notice pain and swelling to stop tissue damage, relieve pain, and decrease swelling.
- After exercise, workouts or activity of any kind to prevent re-injury.
- Before and after surgery during rehabilitation to control pre and post-surgery pain and swelling.
- Anytime you feel your joint has been over-extended, over-worked, twisted, strained or sprained causing pain and swelling.
- Anytime you have swelling, sharp throbbing pain or inflammation.
- Any other situation where you need to draw the pain and inflammation out of the area.
Are You Dealing with Rehabilitation After Bursitis Surgery (Bursectomy)?
Most cases of chronic bursitis injuries will respond VERY well to conservative treatments, however, surgery will be needed in some cases (especially if your bursa needs to be removed). Undergoing bursitis surgery, whether you're having your bursa drained or removed, can be a scary and challenging time for most.
The Internet and any medical professionals available to you (your surgeon, orthopaedic specialist and/or PT) will provide a wealth of information and details on the surgery itself, but it can be a challenge to fully understand the medical terminology used, how your body reacts to the surgery and what comprehensive rehabilitation plan will get your body healed as soon as possible.
Surgery in itself is not the end of the journey, it is merely
the beginning of a new chapter. Your rehabilitation efforts will have an important impact on how soon you can return to living and enjoying your normal daily life.
It truly takes a cohesive rehab plan after surgery - incorporating conservative treatments, rest and PT/exercise - to ensure a complete recovery takes hold. There is no single answer and each individual experience in rehabilitation is different.
Click HERE to Go To Our Online Store If you have questions, call our office at 1-866-237-9608 (toll free continental US).
The Next Step Is Up To You!
Living with pain is never easy as it affects your entire lifestyle. Living with pain during or after intensive surgery with a lengthy rehabilitation period can be even harder! Nothing is more important than making the proper decision when it comes to treating your bursitis and joint pain after surgery.
Doctors and Surgeons are always improving the technologies used in surgery, and results from surgery now are much more positive than they were in the past. However, all surgeries introduce scar tissue, and full recovery from surgery is often less successful than you might expect. If you do wind up getting surgery, know that rehabilitation at-home while attending regular PT or doctor appointments is vital for your overall recovery. It is especially vital to joints that consistently handle extreme forces. Consistent exercise and conservative treatment on a daily basis during your rehabilitation while working with your doctor, surgeon or PT is key.
AidMyBursa stands out in this regard as our goal is to help you recover 100% for the long term during your post-operative rehabilitation and beyond.
We strongly believe that we can help you, and we have thousands of happy clients to back this claim. You are welcome to try our products for a 60 day period.. If you are committed to following the treatments outlined in the product instructions we are very confident that our TShellz Wraps will aid you immensely. If you do not receive the benefits that countless of our other customers have experienced from our products, call us for instructions to mail the product back and we will provide you with a full product refund.

Our online shop accepts Visa & Mastercard as well as a Paypal Payment option.
We also encourage your to Call Our Office at 1-866-237-9608 (toll free continental NA) where we can answer any questions you have and/or take your order via phone.
Ask your PT about the TShellz Wrap® and if it is a suitable treatment option for your recovery! As with all medical devices, make sure your physician is aware of any treatment plan you decide to take. AidMyBursa advisors do not work on commission, so be assured you will only receive fair and objective information.
Learn More About Bursitis Injuries & TreatmentsI want to learn more about Post-Surgery Recovery I want to learn more about TShellz Wrap® Circulatory Boost I want to learn more about Ice & Heat: Which Is Better For Treatment? I want to learn more about Bursitis Treatments I want to learn more about Bursitis Surgery
FREE SHIPPING ON ALL PRODUCTS CURRENTLY ENABLED
60 DAY TRIAL PERIOD
During your recovery, you will probably have to modify and/or eliminate any activities that cause pain or discomfort at the location of your soft tissue injury until the pain and inflammation settle. The more diligent you are with your treatment and rehabilitation, the faster you will see successful results!
| 


















